
All About Breastfeeding. Is It Important? Is It Beneficial?
What is breastfeeding?

Breastfeeding! Is it good for my baby? Is it good for me? Breastfeeding can be such an exciting yet scary experience especially for first-time mothers and mothers-to-be! It is important to know that feeling anxious or scared about the thought of breastfeeding is perfectly normal!
During the first 1-2 hours just after birth, healthy newborns should already be ready and eager to be breastfed. These couple of hours are the most important time for babies not just to be nursed, but also to be with their mothers.
How can I breastfeed effectively?
In order to breastfeed your little one successfully, you will first need to let your baby practice latching on and sucking. Normally, by the second day after birth, your baby should wake up and begin showing signs of readiness for feeding every 1½ to 3 hours making it a total of 8-12 feedings within 24 hours.
Is breastfeeding beneficial for my baby?
Frequent feedings will provide your baby with an abundance of antibody and nutrient-rich first milk (colostrum) that includes:
- Immunoglobins A (an antibody)
- Lactoferrin (type of protein that helps to prevent infections)
- Leukocytes (white blood cells)
- Epidermal growth factor (type of protein that helps to stimulate cell growth)
Colostrum refers to the first milk that forms inside the breasts and plays a vital role in building your baby’s immune system and helps with their growth and development. Colostrum is normally thick and lemon-colored which gradually changes into transitional whitish-yellow breast milk a few days after your baby is born. Colostrum also happens to be rich in protein, low in sugar and full of other beneficial compounds.

Exclusive breastfeeding, meaning to say the baby is only consuming breast milk, is normally recommended by most healthcare professionals for at least the first 6 months of your baby’s life or longer. During these 6 months, breastmilk should contain everything your baby needs. Thus, the composition of the mother’s breast milk will also change in order to match the child’s age and nutritional requirements. Other than that, exclusive breastfeeding can reduce your child’s risk of getting affected by various illnesses and diseases such as:
- Middle ear infections
- Colds and infections
- Respiratory tract infections
- Gut infections
- Intestinal tissue damage
- Sudden Infant Death Syndrome (SIDS)
- Allergic diseases
- Bowel diseases
- Childhood leukemia
- Diabetes (type 1 diabetes and non-insulin-dependent (type 2) diabetes
Furthermore, breastfeeding can also promote healthy weight for your baby. One study done by Grube et al. (2015) discovered that there is a significant reduced likelihood of babies developing obesity and being overweight. Reason behind this could be due to the development of various gut bacteria as breastfed babies have higher amounts of beneficial gut bacteria which could affect the way their fat is stored in their bodies.
In addition, another reason for their healthy weight could be due to the amount of leptin, a hormone that helps to regulate appetite and fat storage in their systems. Lastly, breastfed babies can also self-regulate their milk intake as they are more used to eating until they’re satisfied, which in turn, helps them develop a healthier eating pattern.

Can mothers benefit from breastfeeding too?
Breastfeeding is a wonderful gift from mother to baby. Not only is breastfeeding beneficial for the baby, but also for the mother herself. First and foremost, having a baby can make many mothers feel a sense of fulfillment and joy from the physical touch and emotional connection they experience with their little one when nursing. These feelings can in fact trigger the release of hormones such as:
- Prolactin, to promote milk production along with the development of the mammary glands within the breast tissues.
- Oxytocin, also known as the “love hormone”, is released during and after childbirth and during breastfeeding. This hormone is also know to strengthen physical and emotional bonds between one another. Hence, a mother and her baby through kissing, hugging and cuddling.

Not only that, but breastfeeding can also help to burn extra calories, helping mothers to lose pregnancy weight a little quicker. As mentioned previously that oxytocin is released, it can also help the uterus to return to its pre-pregnancy size and also help to reduce the susceptibility of uterine bleeding in postpartum mothers.
Furthermore, for mothers who have been breastfeeding beyond one year, breastfeeding is also known to help with lowering the risk of developing ovarian and breast cancer and also osteoporosis. The chances of developing postpartum depression is also lower due to the fact breastfeeding can slow down the release of pregnancy hormones rather than abruptly.
Lastly, another benefit for breastfeeding mothers is that it is free and convenient! Mothers, especially those who are traveling or busy would not need to go through the hassle of having to constantly clean out milk bottles and prepare formula for their little ones when on the go.
When should I stop breastfeeding?
According to the World Health Organization, it is recommended that mothers should only be feeding their babies breast milk for the first six months and gradually introduce their baby to age-appropriate solid foods at 6 months and still continue breastfeeding them for at least another 2 years. The term used for stopping breastfeeding is called “weaning” and it is up to a mother and her little one to decide when the time feels right.

What are the positions I can use to breastfeed my baby?
Breastfeeding takes a lot of practice and takes time to find the best and comfortable position for you and your baby. When it comes to breastfeeding, always make sure to have a drink beside you – perhaps a big glass of water to quench your thirst as one breastfeeding session can sometimes take up to an hour! Some of the most popular breastfeeding positions are:
1. The Cradle Hold

Despite this position being one of the most popular breastfeeding positions out there, this may not be the most comfortable position for mothers who had a cesarean birth as it might be quite comfortable having your baby lying across your tummy / incision site. Instead, opt to lay down sideways. For the Cradle Hold, make yourself comfortable by sitting in a comfy chair with armrests or perhaps a bed with pillows and cushions surrounding you.
- Have your baby lie across your lap while facing you.
- Place your baby’s head over your forearm and have their nose facing your nipple.
- Place your baby’s lower arm beneath yours.
- Ensure that your baby’s ear, shoulder and hip are aligned, and not twisted.
2. Lying on your side

Having to breastfeed in the middle of the night, experiencing difficult deliveries or cesarean births are common and normal. Hence, lying on your side is a good alternative when breastfeeding.
- Begin by laying on your side and have your baby laying down with you, facing you. Ensure that your baby’s ear, shoulder and hips are aligned.
- Place some cushions or pillows behind you for extra support. Placing a rolled-up baby blanket behind your baby is also recommended to prevent them from moving around too much – but remember to remove after you’ve finished feeding.
- With the arm you’re lying on, tuck it underneath your head or pillow for extra comfort (without disturbing the position of your baby) and with your other free arm, use it to support and guide your baby to your nipple.
3. Laid-back nursing

Laid-back nursing, also known as “biological nursing” is a type of position where a mother lies back in a comfy semi-reclined position of a sofa or bed. For mothers with cesarean births, have your baby lie across you to avoid contact with your incision site.
- Lie back (not flat) on a semi-reclined sofa or bed.
- Place cushions or pillows to provide more comfort and support to the back, shoulder and neck.
- Place your baby on your front and rest on your tummy. However, if this is uncomfortable for you, lay them to one side.
- While supporting your little one, gently guide them to your nipple.
4. The Rugby Hold / “The Clutch”

This is a good position especially for mothers of twins as you can feed both of them at the same time along with cesarean mothers as there is no pressure on the incision site.
- Sit in a comfy chair with cushions or pillows around you.
- Place your baby at your side, underneath your arm with their hips close to yours.
- Ensure that your baby’s nose is at the same level as your nipple.
- With the palm of your hand, use it to support your baby’s neck
- Gently guide them to your nipple.
When should I seek breastfeeding advice from a medical professional?
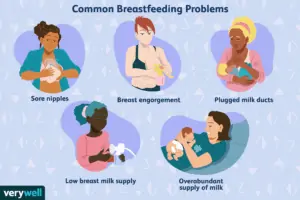 Source: Verywell – Common Breastfeeding Problems
Source: Verywell – Common Breastfeeding Problems
Because mothers want nothing but the best for their children, there is never any harm or shame in seeking advice from a medical professional regarding breastfeeding by seeing their nearest pediatrician, OBGYN or lactation consultant as most, if not all first-time mothers are not fully aware of everything there is to know about breastfeeding. Most mothers are unsure of what to do when they experience difficulties in breastfeeding such as difficult or painful latching, low milk supply, too much milk supply, not knowing whether their baby is satisfied or still hungry or experiencing sore or cracked nipples.
In addition, mothers can also go the nearest pediatric clinic to seek advice and proper physical guidance on how to breastfeed their baby and teach them the right, most comfortable and effective methods and positions for breastfeeding their little ones.
References
Cleveland Clinic. (n.d.). Colostrum.
Grow by WebMD. (n.d.). Breastfeeding.
Grube et al. (2015). Does Breastfeeding Help to Reduce the Risk of Childhood Overweight and Obesity? A propensity Score Analysis of data from the KiGGS Study
Healthline. (n.d.). 11 Benefits of Breastfeeding for Both Mom and Baby.
New York State. (n.d.). Why is Breastfeeding Important for your Baby?
NHS. (n.d.). Breastfeeding: Positioning and Attachment.
Stanford Medicine Children’s Health. (n.d.). Breastfeeding: Getting Start
