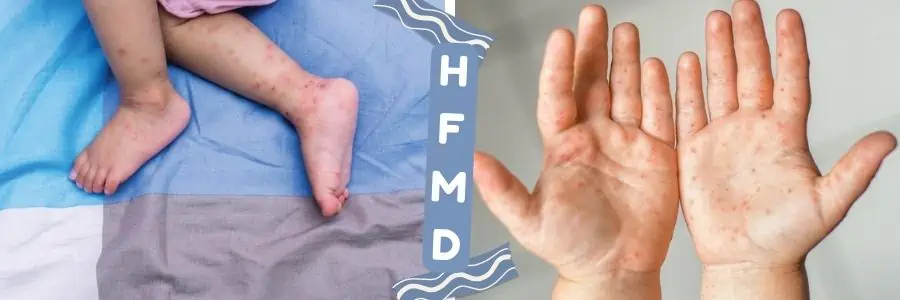
HFMD Explained: All you need to know to protect your little one

In the past few months, we all saw an increase in the prevalance of HFMD in Malaysia. In fact, as of June 14th 2022, the health ministry reported up to 95 000 cases of HFMD, detected between the months of January and June of this year. What was more worrying for parents was that a large majority of those who were infected were children aged 12 and under!
Some parents may have also recently received a call or a note from your child’s day care or school informing you of a reported case of HFMD, or you may have been asked to get your own child checked for the symptoms. To help alleviate some of your concerns and asnwer questions you may have about HFMD, we have combined all the information you need in this article.
Read on further to learn and stay informed on HFMD – including what exactly HFMD is, as well as some tips on the management and prevention of HFMD.
What is HFMD?
HFMD, which is short for hand-foot-and mouth disease, is caused by a group of viruses called enteroviruses. More specifically, HFMD is commonly caused by the coxsackie A16 virus, although other strains of enteroviruses can also cause HFMD.
How can my child get infected?
The main source of infection of the illness is through oral ingestion, meaning that the illness can spread through direct contact with an infected person’s nasal secretions and saliva. Other ways it can spread include direct contact with fluid from an infected person’s blisters, their stool and also from any respiratory droplets in the air after they sneeze or cough.
The virus can also cling to surfaces and remain for several days, which is why it is important to always clean and disinfect toys, utensils and surfaces around the house!
HFMD is a highly contagious illness that can spread very easily and quickly, especially in a day care or school setting, which explains why children are more prone to getting infected. However, more often than not, HFMD is a mild infection that typically subsides within 5-7 days.

Unfortunately, children can get infected by HFMD more than once. Since the illness is brought upon by a virus, the body may build immunity against a particular strain of the virus, but there are many strains that could cause the same infection for the second or third time.
Who can get HFMD?
HFMD is commonly found in children under the age of 5, although older children and teens can also be infected. Of course, adults are also not immune to it. In fact, individuals above the age of 12 accounted for about 2% of the HFMD cases reported by the health ministry this year.
How do I know my child has HFMD?
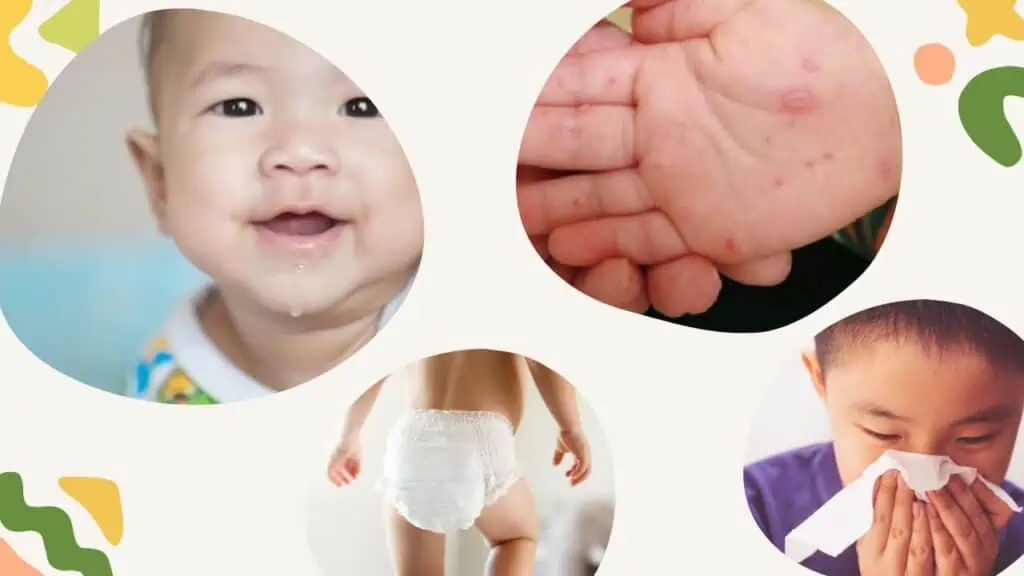
Early symptoms of HFMD resemble a common cold:
- fever
- sore throat
- runny nose
These usually arise 3-6 days after the child has caught the virus.

After a day or two, you may see:
- mouth sores – small painful red spots (herpangina) on the mouth / ulcers on the throat which can become blisters. These can make it difficult/uncomfortable for the child to eat and swallow
- rashes on the skin – flat, red spots on the palms of the hands and soles of the feet. It can also show up on the knees, elbows, buttocks or gential area. Sometimes the rash comes in the form of a blister.
The fluid in the blister usually contains the virus that causes the illness, so try to make sure the child does not touch or pick at the blister.
The spots and rashes are usually not itchy, but can sometimes be painful.

If the child is not eating or drinking, or only prefers to drink cold fluids, it may be a sign that they are finding it painful to swallow.
In rare cases, some complications may arise, such as:
- shortness of breath
- severe headache
- vomiting
- dehydration – if the child is not drinking enough because of the painful mouth ulcers, they could get dehydrated
- encephalitis – in extremely rare cases, individuals with HFMD can get encephalitis (swelling in the brain)
Should I bring my child to see a doctor?
HFMD is a self-limiting disease, meaning that it can usually resolve by itself within a week, so some parents may choose not to bring their child over to see a paediatrician. However, in some cases, it may be better to see a doctor to prevent any further complications.
It is best to see a doctor if the child:
- Has a persisting fever
- Has symptoms that are severe
- Hasn’t recovered from symptoms after 10 days
- Has a weakened/compromised immune system
- Is very young / younger than 6 months
- Does not drink enough fluids to stay hydrated
Signs of dehydration:
- dry mouth
- no tears, sunken eyes
- no wet diaper for 4-6 hours (in infants and toddlers)
- very dark urine, or no urination in 6-8 hours (in older children)
How can I treat / manage HFMD in my child?

- Pain and fever medicine – when it comes to medication, it is best to consult with your paediatrician first, especially if your child is younger than 2 years old. Sometimes, the dosage can depend on the severity of the symptoms, as well as the child’s age and weight. If needed, your child may be prescribed with fever medicine such as paracetamol or ibuprofen. Additionally, you could get a gel or oral spray to help relieve the pain and discomfort caused by ulcers. In this case, take the medication 30 minutes before mealtime to help ease the swallowing of food.
- Staying hydrated – children not getting enough fluids because of the painful mouth sores are at risk of becoming dehydrated. For infants still on breastmilk / formula, offer them more frequent (and possibly smaller) feeds. Older children should be given frequent sips of water, or other liquids such as fruit juice, popsicles or milk.
- Food and meal times – the child’s mouth ulcers can lead to a poor appetite, which in turn can cause them to be lethargic. Offer them foods that are easy to swallow instead, such as mashed potatoes, oatmeal or pureed fruit.
- Rest and sleep – getting enough rest and sleep helps the body to repair and recover. In fact, sleep is just as important as regular exercise and consuming a balanced diet to achieve optimal health and wellness!
How can I prevent HFMD?
As one would expect, prevention of a disease as contagious as HFMD is easier said than done. Nevertheless, here are some ways you can reduce the risk of your child getting infected:
- Frequent hand washing – it is especially important to make sure the hands are clean before the child is eating.
To encourage children to wash their hands, parents can teach them to wash their hands with a song or a video, such as the one in the video below:
Parents must also remember to practice frequent hand-washing, especially after changing diapers, using the toilet, blowing your nose and before/after caring for someone who is ill.
- No sharing of eating utensils, cups, napkins or personal items such as towels and brushes
- Try discouraging older kids from touching their eyes, nose and mouth
- Regularly clean and disinfect toys and surfaces around the house – since babies and toddlers are prone to placing things in their mouth, try to ensure all toys and surfaces around the house are clean
- Avoid close contact with other infected people – this also means that if your child has been diagnosed with HFMD, let them stay at home for a few days and avoid bringing them to crowded places. Usually, it will be safe for them to go out if they 1) have had no fever for 24 hours and 2) any mouth sores, blisters and rashes on the skin have healed
Currently, there are no vaccines that protect against the viruses that cause HFMD, so it is important to practice good hygiene as a way to protect yourself and your children from getting infected.
When can I send my child back to school or day care?
After being diagnosed with HFMD, your child will have been advised to stay at home. Before they can go back to their usual routine, some schools and day care centres require a letter from the doctor to confirm that the child is no longer contagious and has recovered. You can bring your child to a paediatric clinic so that the doctor can check that all the symptoms have cleared up and provide a clearance letter. Usually, the symptoms will take 5-7 days to resolve.
To summarise, hand-foot-and mouth disease is a mild, yet contagious viral infection usually found in young children. As it is a self-limiting disease, it will suually improve on its own within 5-7 days, but sometimes taking medication can help to relieve some pain and discomfort. Remember to consult a doctor first before giving your child medication! Also, to prevent getting infected, practising good hygiene is very important!
On a final note, seeing the number of cases for HFMD rising can cause a lot of anxiety and stress. On top of that, seeing your own child unwell can add to that stress, but try not to worry too much. Keeping your child hydrated and comfortable, and monitoring them for other symptoms is already the best that you can do. In just a few days, your precious little one will be back to their cheery and playful self!
References
CDC. (2022). Hand, Foot, and Mouth Disease (HFMD). https://www.cdc.gov/hand-foot-mouth/index.html
Cleveland Clinic. (2022). Hand, Foot and Mouth Disease: Symptoms, Treatment & Prevention. https://my.clevelandclinic.org/health/diseases/11129-hand-foot-and-mouth-disease
MayoClinic. (2022). Hand-foot-and mouth disease. https://www.mayoclinic.org/diseases-conditions/hand-foot-and-mouth-disease/symptoms-causes/syc-20353035
Murkoff, H. (2022). Hand, Foot and Mouth Disease (Coxsackievirus) in Babies and Toddlers. https://www.whattoexpect.com/first-year/health-and-safety/hand-foot-mouth-disease-coxsackie-virus/
NationWide Children’s. (2022). Hand, Foot and Mouth Disease: Symptoms, Treatment & Prevention. https://my.clevelandclinic.org/health/diseases/11129-hand-foot-and-mouth-disease
Singapore Health. (2022). HFMD: Treatment and Prevention Tips – HealthXchange. https://www.healthxchange.sg/children/health-scares-outbreaks/hfmd-treatment-prevention
